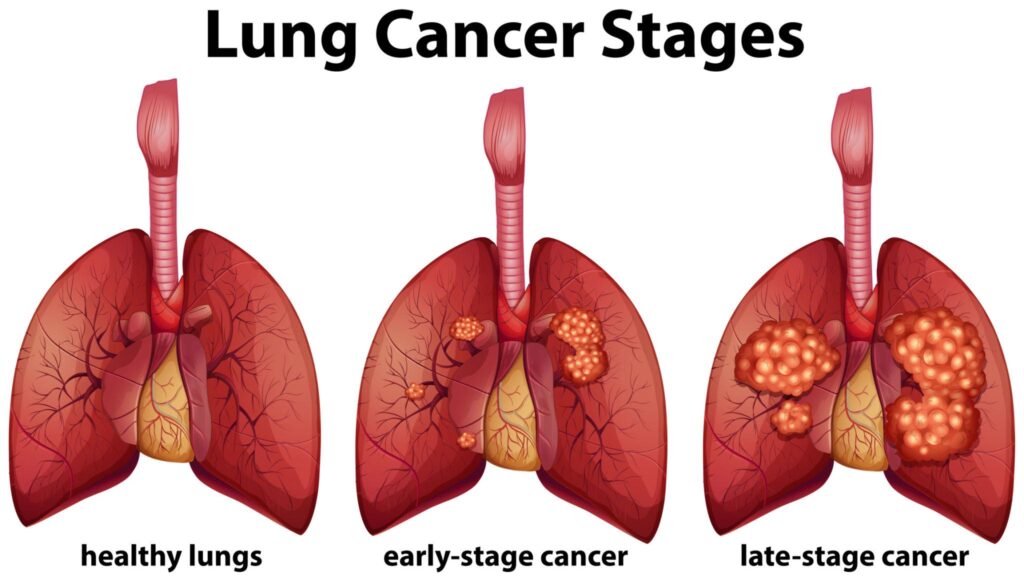
What Is Advanced Stage Lung Cancer?
Understanding Lung Cancer Staging and What It Means
A diagnosis of lung cancer can feel overwhelming—especially when you hear the words advanced stage. But understanding what “advanced stage lung cancer” actually means can help you make informed decisions, ask better questions, and feel more prepared for what lies ahead.
At Stage4Hope, we believe knowledge brings clarity—and clarity brings strength.
What Is Lung Cancer?
Lung cancer begins when abnormal cells grow uncontrollably in the lungs. There are two primary types:
- Non-Small Cell Lung Cancer (NSCLC) – The most common type (about 80–85% of cases)
- Small Cell Lung Cancer (SCLC) – A more aggressive, fast-growing form
Doctors determine how advanced lung cancer is by assigning it a stage. Staging helps guide treatment decisions and gives insight into how far the cancer has spread.
How Lung Cancer Is Staged
Lung cancer is staged using the TNM system, which looks at:
- T (Tumor): Size and location of the main tumor
- N (Nodes): Whether nearby lymph nodes are involved
- M (Metastasis): Whether cancer has spread to distant organs
Stages range from Stage 0 to Stage IV (4).
Lung Cancer Stages Explained
Stage 0 (Carcinoma in Situ)
- Cancer cells are only in the lining of the lung
- No invasion into deeper tissue
- Highly treatable when detected
Stage I
- Cancer is confined to the lung
- No spread to lymph nodes
- Often treated with surgery and possibly chemotherapy
Stage II
- Cancer may have spread to nearby lymph nodes
- Tumor may be larger or invading nearby structures
- Treatment often includes surgery plus chemotherapy
Stage III
- Cancer has spread to lymph nodes in the center of the chest (mediastinum)
- May involve nearby organs or tissues
- Typically treated with a combination of chemotherapy, radiation, targeted therapy, or immunotherapy
Stage III is sometimes referred to as locally advanced lung cancer.
Stage IV (Advanced Stage Lung Cancer)
Stage IV lung cancer is considered advanced stage.
At this stage:
- Cancer has spread (metastasized) beyond the lungs
- Common sites include the brain, bones, liver, or adrenal glands
- It may involve fluid buildup around the lungs (malignant pleural effusion)
Stage IV is further divided into:
- Stage IVA: Cancer has spread within the chest or to one distant organ
- Stage IVB: Cancer has spread to multiple distant organs
While Stage IV is serious, treatment options have advanced significantly in recent years—especially with targeted therapies, immunotherapy, and precision oncology.
What Does “Advanced Stage Lung Cancer” Mean?
“Advanced stage lung cancer” usually refers to:
- Stage III (locally advanced)
- Stage IV (metastatic lung cancer)
It means the cancer has spread beyond its original location and requires comprehensive treatment rather than surgery alone.
However, advanced does not mean untreatable. Many patients live meaningful, extended lives with new treatment breakthroughs, clinical trials, and personalized medicine.
Treatment Options for Advanced Stage Lung Cancer
Treatment depends on cancer type, genetic mutations, overall health, and personal goals. Options may include:
- Targeted therapy (for specific gene mutations like EGFR, ALK, ROS1, RET, KRAS)
- Immunotherapy
- Chemotherapy
- Radiation therapy
- Clinical trials
- Palliative and supportive care
Genetic testing plays a crucial role in advanced lung cancer treatment, helping match patients with therapies designed specifically for their cancer’s biology.
Living With Advanced Lung Cancer
An advanced stage diagnosis affects more than the body—it impacts emotional health, relationships, finances, and daily life.
Patients often face:
- Travel costs for specialized care
- Access barriers to clinical trials
- Emotional strain
- Financial burdens
That’s where support becomes essential.
You Are Not Alone
At Stage4Hope, we exist to improve the lives of advanced-stage cancer patients by:
- Accelerating access to specialized treatments and clinical trials
- Funding cutting-edge precision oncology research
- Providing financial support for treatment-related travel
- Offering free virtual cancer support groups
- Hosting expert-led training and retreats
Whether you’ve just received a diagnosis or have been navigating advanced lung cancer for years, there is strength in community and hope in innovation.
Stay Connected with Stage4Hope
Learn more about advanced-stage lung cancer, treatment breakthroughs, how treatment timing may matter, and living well with Stage 4 cancer. Join our community to receive updates on research, virtual support groups, retreats, and training opportunities designed specifically for those facing late-stage diagnoses.
You don’t have to walk this journey alone.
Does Treatment Timing Matter in Lung Cancer?
Does Immunotherapy Treatment Timing Matter in Lung Cancer?
Could Timing Give Your Cancer Treatment a Boost?
A new clinical trial is sparking real conversation in the lung cancer community by asking a surprisingly simple question: Does the time of day you receive treatment affect how well it works? For people living with advanced non-small cell lung cancer (NSCLC), this research offers a hopeful — and low-cost — idea that could one day improve outcomes without changing the drugs themselves.
Morning vs. Afternoon Immunotherapy for Lung Cancer
In a randomized clinical trial, researchers found that patients who received immunochemotherapy earlier in the day lived longer and had better control of their cancer compared to those treated later in the afternoon. Immunochemotherapy is a combination of immunotherapy (which helps your immune system recognize and attack cancer) and chemotherapy (which directly kills cancer cells). Patients treated earlier had a 60% lower risk of cancer progression and a 48% lower risk of early death.
What the Study Found — In Plain Language
The phase 3 LungTIME-C01 trial followed 210 people with advanced (stage IIIC or stage 4) non-small cell lung cancer who did not have known genetic driver mutations. Everyone received the same drugs — the only difference was when treatment was given:
-
Early group: Treatment before 3:00 PM
-
Late group: Treatment after 3:00 PM
After more than two years of follow-up, the differences were striking:
-
Cancer stayed under control for about 11 months in the early-day group
-
Cancer worsened in about 6 months for those treated later
-
Overall survival was 28 months vs. 16.8 months, favoring earlier treatment
Researchers believe this benefit may be tied to the body’s circadian rhythm — the natural 24-hour cycle that regulates hormones, immune activity, and cell behavior.
Why the Immune System’s “Clock” Matters
Your immune system doesn’t work the same way all day long. Certain immune cells — especially CD8+ T cells, often called “killer” T cells — appear to be more active and effective earlier in the day.
In this study, patients treated in the morning had:
-
More circulating CD8+ T cells
-
A healthier balance of activated (ready to fight cancer) vs. exhausted immune cells
This may explain why immunotherapy worked better earlier in the day — the immune system was simply more prepared to respond.
Should Patients Change Their Treatment Time Now?
Not yet — and that’s important to say clearly.
While many experts find the results exciting, others urge caution. This is the first randomized trial to confirm what earlier observational studies only suggested. Larger studies and reviews of past trials are still needed before treatment timing becomes part of standard care.
That said, this approach is especially intriguing because:
-
It doesn’t add new drugs
-
It doesn’t increase toxicity
-
It could be easier to implement than many medical advances
Some researchers believe timing may matter most during the first cycle of immunotherapy, when the immune system is being “trained” to recognize cancer.
What This Means for Patients Today
If you’re receiving or considering immunochemotherapy:
-
Timing is not part of standard treatment guidelines yet
-
This study is promising, but still early
-
It may be worth asking your oncologist whether infusion timing is flexible — especially at the start of treatment
As always, treatment decisions should be personalized, balancing science, logistics, and what’s realistic for you.
At Stage4Hope, we believe progress often comes from unexpected places — and sometimes, hope comes from asking new questions about familiar treatments. We’ll continue to follow this research closely and share updates as more data becomes available.
Questions to Ask Your Doctor
-
Does treatment timing matter for my specific cancer?
-
Is morning treatment an option for me?
-
How does immunotherapy work with my immune system?
-
What side effects should I watch for?
Stay Connected with Stage 4 Hope
AI in Lung Cancer Treatment
How AI Is Improving Lung Cancer Treatment: New Tools, Real Impact
See how AI is helping guide immunotherapy decisions, combine imaging for deeper insights, and support earlier detection—bringing more personalized lung cancer care.
Three Ways AI Is Moving Lung Cancer Care Forward
1) AI that predicts immunotherapy response in advanced NSCLC (Deep-IO)
A validated deep-learning model called Deep-IO may help doctors better predict which patients with advanced non-small cell lung cancer (NSCLC) will respond to immunotherapy—using routine pathology slides from tumor biopsies. In the study discussed in a Physician’s Weekly Q&A, researchers trained the model on hundreds of thousands of image “tiles” from 958 patients (US + EU cohorts, 2014–2022). The model showed meaningful accuracy for predicting response (reported AUCs varied by cohort) and, importantly, it may help identify non-responders more specifically—potentially sparing patients ineffective treatment and side effects. The article also notes that combining Deep-IO + PD-L1 performed better than either marker alone in that validation setting.1
2) “Connecting the dots” across cancer images (Emory)
A separate Emory report highlights how AI is being used to combine different kinds of cancer images—from microscopic tissue slides to CT scans and even epigenetic data—so researchers can build a more complete picture of how a tumor behaves. In four studies (focused on head and neck cancers), one team used an AI platform called VISTA to transform standard H&E slides into “virtual IHC” to help identify tumor-associated macrophages that are otherwise difficult to see. Another approach adapted a swin transformer into a multimodal framework (called SMuRF) that helped integrate 2D pathology images with 3D radiology, supporting predictions about survival and even which patients might benefit from chemotherapy. A fourth effort linked slide images with epigenetic patterns using pathogenomic fingerprinting, aiming to improve risk assessment. Emory’s researchers also emphasize the need to be cautious and thoughtful before moving these tools fully into clinical practice.2
3) What this means for lung cancer patients right now
Together, these developments point to a near-future where AI can support:
- More personalized treatment selection (who is most likely to benefit from immunotherapy)3
- Smarter risk and prognosis tools by combining radiology + pathology + other data4
- Earlier detection and faster pathways to care, especially as imaging AI expands in real-world settings5
It’s also important to keep the balance: experts continue to flag challenges like bias and fairness, the need for diverse multi-site datasets, and careful clinical validation before widespread adoption.6
More examples of AI in cancer research and care
- NCI’s HistoTME model (NSCLC + immunotherapy): An NCI team described HistoTME, which analyzes digital pathology images to learn about the tumor microenvironment and improve prediction of immunotherapy response—supporting biomarker discovery and more personalized immunotherapy strategies.7
- AI-driven early lung cancer detection (Bristol Myers + Microsoft, Jan 20, 2026): Reuters reports a collaboration using FDA-cleared radiology AI algorithms through Microsoft’s Precision Imaging Network to help clinicians detect lung nodules earlier and expand access in underserved communities.8
- AI + breast cancer screening at scale (EDITH trial, UK): A UK government announcement describes a large NHS trial (~700,000 participants) evaluating AI to support mammogram reading and potentially reduce the need for a second specialist reader.9
- Multimodal AI for recurrence risk (AACR, Dec 10, 2025): AACR describes an AI model combining digitized pathology slides with molecular + clinical data to improve long-term recurrence risk stratification in early breast cancer.10
- AI to speed oncology drug research (AstraZeneca + Modella AI, Jan 13, 2026): Reuters reports AstraZeneca agreed to acquire Modella AI to boost quantitative pathology and biomarker discovery for oncology R&D.11
AI is a supportive tool
AI isn’t replacing oncologists—it’s becoming a powerful support tool that can help doctors see patterns humans can’t easily spot, match patients to therapies more precisely, and potentially reduce trial-and-error in treatment. If you or someone you love is living with lung cancer, it may be worth asking your care team about biomarker testing (like PD-L1), available clinical trials, and how new imaging or pathology tools are shaping treatment decisions.12
Resources for Living With Stage 4 Cancer
Whether you’re navigating treatment options, seeking emotional support, or trying to make sense of a new diagnosis, Stage 4 Hope is here for you. Become a member of our community to gain access to trusted resources, as well as online support and more.
References:
- https://www.physiciansweekly.com/post/qa-validated-ai-model-could-guide-real-world-nsclc-decisions
- https://news.emory.edu/stories/2025/06/hs_head_and_neck_16-06-2025/story.html
- https://www.physiciansweekly.com/post/qa-validated-ai-model-could-guide-real-world-nsclc-decisions
- https://news.emory.edu/stories/2025/06/hs_head_and_neck_16-06-2025/story.html
- https://www.reuters.com/business/healthcare-pharmaceuticals/bristol-myers-partners-with-microsoft-ai-driven-lung-cancer-detection-2026-01-20/
- https://www.cancer.gov/about-nci/organization/cbiit/news-events/news/2025/artificial-intelligence-ai-model-histotme-aids-predicting-response-immunotherapy
- https://www.reuters.com/business/healthcare-pharmaceuticals/bristol-myers-partners-with-microsoft-ai-driven-lung-cancer-detection-2026-01-20/
- https://www.gov.uk/government/news/world-leading-ai-trial-to-tackle-breast-cancer-launched
- https://www.aacr.org/about-the-aacr/newsroom/news-releases/a-multimodal-ai-model-may-improve-recurrence-risk-stratification-in-early-breast-cancer/
- https://www.reuters.com/business/healthcare-pharmaceuticals/bristol-myers-partners-with-microsoft-ai-driven-lung-cancer-detection-2026-01-20/
- https://www.physiciansweekly.com/post/qa-validated-ai-model-could-guide-real-world-nsclc-decisions
Lung Cancer in Nonsmokers
Lung Cancer in Nonsmokers: The Truth, the Science, and Stories of Hope
Lung cancer is often treated like a “smoker’s disease,” but that stereotype is outdated—and it’s hurting people. Many patients have never smoked, and women under 65 are now seeing higher incidence rates than men in some age groups. What’s behind these cases? Often, the answer is biology: genetic mutations that can drive lung cancer even without traditional risk factors.
In this post, we’ll cover what’s driving lung cancer in nonsmokers (including RET-positive lung cancer and EGFR mutations), why stigma matters, what genetic testing can uncover, and how real patients are finding hope through research, advocacy, and community.
The Truth About Lung Cancer: It’s Not Just a Smoker’s Disease1
Lung cancer still carries a painful stigma. Many patients report feeling blamed or judged—by friends, family, and even medical professionals—because people assume smoking caused their disease. But anyone with lungs can get lung cancer, and no one deserves to be blamed for a diagnosis.
That stigma can do real harm. It’s been associated with delayed care, higher rates of depression, and lower screening rates—despite the fact that screening can catch lung cancer earlier, when treatment is often more effective. Shifting the narrative matters: lung cancer is a health issue, not a moral failing.
Lung Cancer in Women and Nonsmokers: What to Know2
Lung cancer diagnoses are declining overall, but a growing number of cases are being found in people who don’t fit the “typical” image—especially younger women and nonsmokers.
One reason some cases are missed or delayed is misdiagnosis. Younger nonsmoking women are sometimes told symptoms are asthma, bronchitis, or allergies, which can cost precious time. If you feel something is wrong, trust yourself. Persistent symptoms deserve follow-up, regardless of age or smoking history.
What’s Driving Lung Cancer in Nonsmokers?3
For many nonsmokers, lung cancer is driven by genetic mutations—changes inside cancer cells that help tumors grow. These are not the same as inherited risk (though inherited factors can play a role). Instead, they’re often tumor biomarkers that guide treatment.
This is why genetic testing (also called biomarker testing or molecular testing) is so important—especially for people with advanced lung cancer. It helps doctors match a patient to targeted therapy, which may be more effective and sometimes better tolerated than standard approaches alone.
Understanding RET-Positive Lung Cancer
One mutation that can drive lung cancer in nonsmokers is a RET fusion. RET-positive lung cancer is more common in never-smokers and can occur in younger patients, including women. It also may not show up through routine screening, which makes awareness and appropriate testing even more important.
Why it matters: If a tumor is RET-positive, a patient may be eligible for targeted treatments designed specifically to block RET-driven cancer growth. That can change the entire treatment plan—and outcomes.
Takeaway: If you or a loved one is diagnosed with lung cancer—especially stage 4 or hard-to-treat disease—ask your care team about biomarker testing early.
(Source: American Cancer Society, Yale Medicine, J Clin Oncol)
Read the complete article here
EGFR and Other Mutations: Why Testing Can Change Everything5
Mutations like EGFR are also more common in women and are seen at higher rates in certain populations, including Asian women. These biomarkers can open the door to targeted therapies that are specifically designed for cancers driven by those mutations.
The bottom line: lung cancer treatment is becoming more personalized. But personalization starts with testing.
How Research Is Accelerating Answers: The Lung Cancer Genetics Study6
A powerful genetics study is bringing hope to people facing lung cancer—especially nonsmokers and those with rare mutations. The Lung Cancer Genetics Study is collecting patient genetic and clinical data to help researchers:
- identify patterns in lung cancer among nonsmokers
- accelerate discoveries for rare mutations
- support more personalized treatment approaches
As more people participate and more data becomes available, researchers can move faster—and patients benefit from better-informed care.
Lung Cancer in Non-Smokers: Survivor & Patient Stories
Scientific progress matters—but so do stories. Real people are living proof that the lung cancer narrative is bigger than stigma.
From Remission to Recurrence: Karen’s Stage 4 Lung Cancer Journey
Karen was diagnosed with lung cancer at 47—a healthy, never-smoker with no family history—and after surgery, chemo, and eight clear years of scans, her cancer returned and became stage 4. Strengthened by new breakthroughs in lung cancer research, she continues to live fully. Karen’s story is a reminder that advances in treatment are giving patients more options, more time, and more hope.
Stage 4 Lung Cancer Veteran: Xavier Fights for Awareness
Air Force veteran Xavier Sanders was diagnosed with stage 4 lung cancer despite never smoking. He’s raising awareness about burn pit exposure, early detection, and support for service members. He’s not just fighting for himself. Xavier is advocating for younger airmen who may not know what symptoms to watch for or how to get the right care.
What You Can Do: Advocate for Yourself or Someone You Love
If you’re concerned about symptoms or navigating a diagnosis, these steps can help:
- Don’t dismiss persistent symptoms—especially a cough that won’t go away, shortness of breath, chest pressure, or unexplained weight loss
- Ask about lung cancer screening if you’re eligible
- If diagnosed, request biomarker testing early (RET, EGFR, and other drivers)
- Ask your doctor about targeted therapy, immunotherapy, and clinical trials when appropriate
- Seek community—support improves coping, confidence, and follow-through with care
You’re Not Alone—Connect with the Stage 4 Hope Community
Whether you’re navigating treatment options, seeking emotional support, or trying to make sense of a new diagnosis, Stage 4 Hope is here for you. Learn more about topics like lung cancer in nonsmokers by joining our community. Connect with others who understand your experience and gain access to trusted resources, medical updates, and invitations to supportive virtual gatherings.
References:
- https://www.mskcc.org/news/understanding-stigma-lung-cancer
- https://www.mskcc.org/news/lung-cancer-in-women-and-nonsmokers-what-to-know-about-symptoms-diagnosis-and-treatment
- https://happylungsproject.org/lung-cancer-risk-factors-understanding-its-causes-and-prevention/
A New Cancer Therapy: Exercise
How Exercise May Help Improve Energy, Brain Function, and Recovery During and After Cancer Treatment
Many people facing cancer treatment are told to rest—and while rest is important, research is showing something surprising:
Exercise may be one of the most powerful tools to support recovery during and after cancer treatment.
In fact, new research suggests that movement doesn’t just improve energy and strength—it may even play a role in how the body responds to cancer itself.
What Cancer Patients and Astronauts Have in Common
New cancer patients may be surprised to learn they share something in common with astronauts in space.
According to researchers at Memorial Sloan Kettering, the effects of inactivity during cancer treatment can be similar to what astronauts experience in zero gravity. Both can lead to:
- Loss of muscle strength
- Reduced cardiovascular fitness
- Changes in brain function
NASA researchers even use the term “space fog”—a condition that closely resembles what cancer patients often call chemo brain.
What Is Chemo Brain (Chemo Brain Fog)?
Chemo brain, also called chemo brain fog, refers to cognitive changes that can happen during or after cancer treatment.
People often describe it as:
- Difficulty concentrating
- Memory problems
- Trouble finding the right words
- Mental “slowness” or fogginess
These symptoms can be frustrating and may affect work, relationships, and daily life.
Chemo brain is not just “in your head.” It is a real and recognized side effect of cancer treatment, likely caused by a combination of:
- Chemotherapy effects on the brain
- Inflammation
- Fatigue
- Stress and emotional strain
How Long Does Chemo Fatigue Last?
Fatigue is one of the most common side effects of cancer treatment.
For many people:
- Fatigue begins during treatment
- It may continue for weeks or months afterward
- Some experience longer-term fatigue, especially after intensive treatment
Unlike normal tiredness, chemo fatigue does not always improve with rest alone. This is where new research is changing the conversation.
How to Regain Energy After Chemotherapy
It may seem counterintuitive, but one of the most effective ways to regain energy after chemotherapy is through gentle, consistent movement.
Research shows that exercise can:
- Improve energy levels
- Reduce fatigue
- Support heart and lung function
- Help rebuild muscle strength
- Improve mood and mental clarity
Even small amounts of movement—like walking a few times a week—can make a meaningful difference.
A Shift in Thinking: Exercise as Therapy
Contrary to popular belief, the best way to recover from cancer treatment is not always to stay in bed.
Exercise physiologists at Memorial Sloan Kettering emphasize that:
- Regular movement improves both physical and mental health
- Exercise helps reduce long-term side effects of treatment
- Patients who exercise experience less decline in overall fitness
In one study, people undergoing chemotherapy experienced a 15% drop in fitness levels, similar to a decade of aging—but exercising just three times per week significantly reduced that decline.
Exercise Guidelines for Cancer Survivors
While every person’s situation is different, general exercise guidelines for cancer survivors often include:
- Start slow and build gradually
- Aim for light to moderate activity (like walking)
- Work toward 150–225 minutes per week, if possible
- Include both aerobic activity and strength training
- Listen to your body and rest when needed
It’s always best to speak with your care team or an exercise specialist before starting a new routine.
Can Exercise Help Chemo Brain?
Emerging research suggests that exercise may also help improve cognitive function.
Chemo Brain Exercises That May Help:
- Walking or light cardio (improves blood flow to the brain)
- Strength training (supports brain-body connection)
- Balance and coordination exercises
- Mind-body practices like yoga
Exercise may help:
- Improve focus and attention
- Support memory function
- Reduce mental fatigue
This is one of the reasons researchers are studying exercise not just as recovery—but as a form of therapy.
A Groundbreaking Clinical Trial on Exercise and Cancer
In a first-of-its-kind clinical trial, researchers studied how different “doses” of exercise affected men with prostate cancer before surgery.
Participants were assigned structured exercise plans ranging from:
- 90 minutes per week
- Up to 450 minutes per week
The results were surprising.
Most of the benefit occurred at 225 minutes per week (about 3 hours and 45 minutes)—with no added benefit beyond that level. This challenges the idea that more exercise is always better.
Can Exercise Affect Cancer Itself?
Researchers are now exploring whether exercise can do more than improve symptoms.
Early evidence suggests exercise may:
- Influence tumor biology
- Improve how treatments work
- Potentially slow cancer progression
While more research is needed, this opens the door to a new concept:
Exercise as part of cancer treatment—not just recovery.
Finding a Sense of Control During Cancer
For many patients, exercise provides something just as important as physical benefits—a sense of control.
During a time when so much feels uncertain, movement can be:
- A daily routine
- A personal goal
- A way to actively participate in your healing
As one patient shared, exercise became something “100% under my control” during treatment.
Why This Matters
This research is changing how we think about cancer care.
Instead of focusing only on treatment, there is growing recognition that:
- Supporting the whole body matters
- Recovery is active, not passive
- Small, consistent steps can lead to meaningful improvements
Exercise is not a cure—but it is a powerful tool.
(Source: Memorial Sloan Kettering News- 2025, Issue 1)
Resources for Living With Stage 4 Cancer
Learn more about topics like exercise and cancer treatment, along with other important aspects of living with Stage 4 cancer. Become a member of our community to gain access to trusted resources, online support and education from Dr. Sharon May, Ph.D., LMFT, medical updates, and invitations to supportive virtual gatherings.